Get Full Access with a FREE Account
- Latest medical news
- Peer-reviewed clinical content
- Conference coverage
- Free CME/CE
- Quizzes to test your knowledge
- Research summaries
Latest News
May 9, 2024
Genes May Govern Intestinal Sites of Pediatric Crohn’s
May 9, 2024
GI and Hepatology News
May 9, 2024
Negative Colonoscopy? 15-Year Screening Interval May Be Safe
May 9, 2024
MDedge Hematology and Oncology
May 9, 2024
Clinical Guidelines: Start Screening at Age 50 for Age-Related Hearing Loss
May 9, 2024
MDedge Family Medicine
May 9, 2024
Pediatrician Credibility Remains Intact in Midst of Health Misinformation
May 9, 2024
PAS: Pediatric Academic Societies
MDedge Pediatrics
Photo Challenge
April 29, 2024
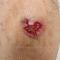
Chronic Cribriform Ulcerated Plaque on the Left Calf
April 29, 2024
MDedge Dermatology

April 16, 2024
Progressively Worsening Scaly Patches and Plaques in an Infant
April 16, 2024
MDedge Dermatology
Clinical Reviews
May 6, 2024
An Update on Cutaneous Angiosarcoma Diagnosis and Treatment
May 6, 2024
MDedge Dermatology

April 25, 2024
Dermatologic Care for Refugees: Effective Management of Scabies and Pediculosis
April 25, 2024
MDedge Dermatology

April 8, 2024
Evaluating the Cost Burden of Alopecia Areata Treatment: A Comprehensive Review for Dermatologists
April 8, 2024
MDedge Dermatology
March 5, 2024
Depression As a Potential Contributing Factor in Hidradenitis Suppurativa and Associated Racial Gaps
March 5, 2024
MDedge Dermatology
Coronavirus Updates
April 24, 2024
Federal Trade Commission Bans Noncompete Agreements, Urges More Protections for Healthcare Workers
April 24, 2024
MDedge Infectious Disease
April 18, 2024
COVID Vaccinations Less Prevalent in Marginalized Patients
April 18, 2024
MDedge Infectious Disease
April 18, 2024
4 Years In, a Sobering Look at Long COVID Progress
April 18, 2024
MDedge Infectious Disease
April 5, 2024
Study Shows Nirmatrelvir–Ritonavir No More Effective Than Placebo for COVID-19 Symptom Relief
April 5, 2024
MDedge Infectious Disease
Business of Medicine
May 9, 2024
Pediatrician Credibility Remains Intact in Midst of Health Misinformation
May 9, 2024
PAS: Pediatric Academic Societies
MDedge Pediatrics
May 9, 2024
Plastic Surgeon Illegally Restricted Negative Reviews, Judge Rules
May 9, 2024
MDedge Dermatology
May 8, 2024
Docs Vent As Feds Investigate Private Equity, Consolidation in Medicine
May 8, 2024
MDedge Internal Medicine

May 8, 2024
Consider a Four-Step Approach to Shared Decision-Making in Pediatric Dermatology
May 8, 2024
AAD: American Academy of Dermatology
MDedge Dermatology
May 7, 2024
Do Health-Related Social Needs Raise Mortality Risk in Cancer Survivors?
May 7, 2024
MDedge Hematology and Oncology
Conference Coverage
May 9, 2024
Pediatrician Credibility Remains Intact in Midst of Health Misinformation
May 9, 2024
PAS: Pediatric Academic Societies
MDedge Pediatrics
May 9, 2024
For Pediatric LGS, Cenobamate Shows Promise
May 9, 2024
AAN: American Academy of Neurology
MDedge Neurology
May 9, 2024
Diabetes/Weight Loss Med Linked to Repeat Spinal Surgery
May 9, 2024
MDedge Internal Medicine

May 9, 2024
Diacerein, Resveratrol, Botulinum Toxin Disappoint in Knee Osteoarthritis
May 9, 2024
OARSI: OsteoArthritis Research Society International
MDedge Rheumatology
Medicine's Lighter Side

June 15, 2023
The road to weight loss is paved with collusion and sabotage
June 15, 2023
MDedge Internal Medicine
Perspectives
May 7, 2024
Comment on “Skin Cancer Screening: The Paradox of Melanoma and Improved All-Cause Mortality”
May 7, 2024
MDedge Dermatology
Clinical Edge Journal Scan

May 9, 2024
Genes May Govern Intestinal Sites of Pediatric Crohn’s
May 9, 2024
GI and Hepatology News
May 9, 2024
Negative Colonoscopy? 15-Year Screening Interval May Be Safe
May 9, 2024
MDedge Hematology and Oncology
May 9, 2024
Clinical Guidelines: Start Screening at Age 50 for Age-Related Hearing Loss
May 9, 2024
MDedge Family Medicine
May 9, 2024
Pediatrician Credibility Remains Intact in Midst of Health Misinformation
May 9, 2024
PAS: Pediatric Academic Societies
MDedge Pediatrics







